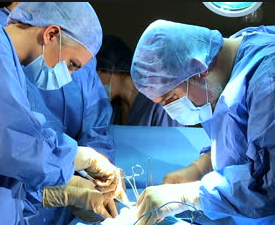
 Doctors and researchers at MD Anderson are exploring hypnosedation to manage pain and anxiety during certain breast cancer surgeries.
Doctors and researchers at MD Anderson are exploring hypnosedation to manage pain and anxiety during certain breast cancer surgeries.
When Beverly Levinson’s doctor noticed two unusual spots on her dense breasts, she was sent to The University of Texas MD Anderson Cancer Center for a lumpectomy—a surgical procedure to remove abnormal or cancerous tissue along with a small portion of the surrounding healthy tissue.
Levinson, 64, wasn’t as concerned about the surgery as she was about undergoing general anesthesia. She had received general anesthesia for previous surgeries, but because of her temporomandibular joint (TMJ) disorder, she suffered severe jaw pain from opening her mouth wide enough for the breathing tube to be inserted down her throat.
Luckily, an unconventional solution presented itself to Levinson. Her surgeon approached her about an ongoing clinical trial that would allow her to avoid general anesthesia by using hypnosis. Levinson, who had been hypnotized for jaw pain years ago, immediately jumped at the opportunity.
“In my eyes, I had nothing to lose,” Levinson said. “I could try something new or I could go the old-fashioned way. I’m the middle child. I always try new things. That’s my personality.”
Led by Lorenzo Cohen, Ph.D., director of the Integrative Medicine Program at MD Anderson, the ongoing clinical trial aims to determine whether or not a method of deep relaxation, called hypnosedation, is safe and effective for patients with stage 0/1 breast cancer who are undergoing lumpectomies with or without sentinel lymph node dissections.
The study, still in its pilot phase, will examine 50 patients who are randomly selected to receive either general anesthesia or a combination of local anesthesia and hypnosedation before and during surgery.
In both cases, a patient has an intravenous line placed in her arm and an anesthesiologist is present to administer a cocktail of drugs used to put her under.
For patients receiving hypnosis, the anesthesiologist monitors their vitals, calculates the appropriate dose of local anesthetic medication, administers medication for pain and nausea and stands by to convert to general anesthesia if the patient experiences any discomfort.
“Over the past couple of decades there is a very solid evidence base that incorporating hypnosis during invasive conscious sedation medical procedures reduces  anxiety, helps to control pain, decreases recovery time, and helps lower medical costs,” Cohen said.
anxiety, helps to control pain, decreases recovery time, and helps lower medical costs,” Cohen said.
General anesthesia is still the standard approach at MD Anderson, even for smaller surgeries, such as lumpectomies. But the drugs used for general anesthesia can potentially weaken the body’s immune system and slow the recovery process, Cohen said.
Cancer patients, in particular, cannot afford to have their immune systems compromised. Cohen and his team want to find out if hypnosedation would be a viable replacement for general anesthesia during smaller, less invasive surgeries.
The practice of hypnosis, in one form or another, has been around for centuries. But it wasn’t until the mid-19th century that it came to be defined as a kind of “nervous sleep” that could alleviate anxiety or pain during medical procedures.
In the 1840s, Scottish neurosurgeon James Braid developed a technique of deep relaxation and visual fixation to guide patients into a trance and help alleviate their pain.
He coined the term “hypnosis” and defined it as “the induction of a habit of abstraction or mental concentration, in which … the powers of the mind are so much engrossed with a single idea or train of thought, as … to render the individual unconscious of, or indifferently conscious to, all other ideas, impressions, or trains of thought.”
Although hypnosis is often associated with parlor tricks and stage magicians, the practice itself has been used clinically to address several conditions, including smoking, anxiety and overeating.
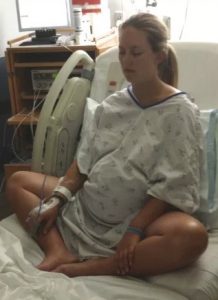
For Levinson, it was a great option. A week before surgery, Levinson met with Rosalinda Engle, a mind-body specialist at MD Anderson Cancer Center who would perform the hypnosedation, in a small conference room in the hospital.
 “Do you have a place where you feel really comfortable and at ease?” Engle asked Levinson in her soothing, mellifluous voice. “It could be your grandmother’s house.
“Do you have a place where you feel really comfortable and at ease?” Engle asked Levinson in her soothing, mellifluous voice. “It could be your grandmother’s house.
It could be a vacation you’ve enjoyed, a vacation spot. It could be anywhere, any place in nature. Close your eyes and call that up.”
As Levinson focused on the task, Engle continued to offer instruction.
“Breathe in deeply. Experience your breath from the tip of your nose. Feel as your breath moves through your body. Imagine breathing into the palm of your hands. Now exhale. Breathe out through your fingers, the soles of your feet, your toes. Relax.”
Slowly but surely, Engle lulled Levinson into a state of deep relaxation.
“I felt very, very safe,” Levinson said, when it was over. “It was like [going] into someone’s house where they’re baking a cake. It smells good, and they welcome you in. You just have a warm feeling.”
Engle guided Levinson through what to expect on the day of the surgery. The room would be sterile, with five or six people at hand. The lights would be bright. Engle would sit beside her throughout the procedure to keep her calm and relaxed.
“My sole job is to sit at the head of the bed and focus on the patient,” Engle said. “Any changes to breathing patterns [or] facial muscles will alert me that I need to check in. Periodically, I’ll ask the patient, ‘How’s your comfort level?’”
On the day of the surgery, doctors injected local anesthetics— lidocaine and bupivacaine—to numb Levinson’s right breast and made a 1-inch incision to remove some of the tissue.
As promised, Engle sat next to Levinson for the duration of the surgery, helping her maintain a state of deep relaxation.
“I didn’t feel anything,” Levinson said. “You’re in a calm state. You’re in a safe state of mind. You’re being reassured. It was great.”
Throughout the surgery, Levinson recalled feeling pressure on her breast as the surgeon operated, but said it didn’t hurt any worse than getting a filling at the dentist.
Less than an hour after her surgery was complete, Levinson was out of bed, dressed and walking around. She skirted the unpleasant side effects of general anesthesia, recovered faster and didn’t require any post-operative painkillers.
For hypnosedation to work, Engle said, the patient must be receptive to it.
“All hypnosis is self-hypnosis,” Engle said. “You’ll go as deep into this trance state as you are willing to allow yourself to go.”
Engle points to shifts in attention and consciousness that people commonly experience throughout the day. Ordinary moments—such as zoning out while driving or becoming so engrossed in a conversation that you’re able to block out surrounding noise—are examples of how the mind can tune out distractions.
“Pointing out these everyday shifts and our capacity for absorption is important to let the patients know they are in control and driving this experience,” Engle said. “They can train themselves to be as relaxed and calm as possible.
 They can guide themselves. They can walk through this experience with surgery and take it throughout the treatment process, the whole continuum of cancer care.”
They can guide themselves. They can walk through this experience with surgery and take it throughout the treatment process, the whole continuum of cancer care.”
While general anesthesia is very safe for most people, it can have unpleasant side effects. The most common are temporary nausea and vomiting, dry mouth, a sore throat and grogginess.
Older patients who receive general anesthesia are more likely to experience longer-term cognitive and memory impairments, a condition called post-operative cognitive dysfunction (POCD) that can last anywhere from a few days to a few months. Those with a history of POCD have a higher risk of experiencing the condition again with repeated anesthetic.
“[Hypnosedation] is a nice alternative,” said Elizabeth Rebello, M.D., associate professor in the department of anesthesiology and perioperative medicine at MD Anderson. “The patient doesn’t require an extended period of time in the recovery room. They’re able to go on with the rest of their life.”
According to Cohen, more than 34 clinical trials and numerous papers published in scientific journals have shown that hypnosedation works. But he says there is still some doubt among his colleagues.
“Although a physician may think, ‘I don’t believe in hypnosis,’ that is a scientifically unsound statement. Science is not about personal belief. It’s about evidence,” Cohen said.
“Your religious practices are part of a belief system. Science is evidence-based. Unfortunately, there are some people who approach science from a belief perspective, as well, and they’re wrong.”
Most surgeons were initially reluctant to participate in the clinical trial, said Dalliah M. Black, M.D., a breast surgical oncologist at MD Anderson.
Because the standard approach at MD Anderson is to use general anesthesia for surgeries large and small, most surgeons are accustomed to having their patient sleep throughout every procedure.
“Surgeon interest was very slow up front, but I would offer them to come in to watch my cases,” Black said. “Many colleagues have been so surprised.”
Using hypnosedation, patients like Levinson can gain some semblance of control during an otherwise stressful experience.
“It’s amazing how complex we are as humans and how complex the mind is. A lot of times, it’s mind over matter,” Black said. “Hypnosedation is a way we’ve applied mind over matter to a situation in the operating room for a specific population of the patients here.
That mental fortitude and the strength that we have, that has to be carried through and has better outcomes if we use that path throughout our cancer care.”
No matter how effective the clinical trial shows hypnosedation to be for surgeries, Rebello stressed that hypnosedation will not become a new standard approach for pain management.
“I think there’s a concern that this is going to replace general anesthesia. It is not going to replace general anesthesia,” Rebello said. “But for a certain niche of patients, there are certainly some benefits that could exist and we need to find out if that is, indeed, the case.
By: Shanley Pierce

 Last summer, at age 14, Sue Jones suffered from stabbing pains in her abdomen that got so intense, “I couldn’t walk.”
Last summer, at age 14, Sue Jones suffered from stabbing pains in her abdomen that got so intense, “I couldn’t walk.”
She spent three weeks in a wheelchair while doctors ruled out everything from digestive problems to appendicitis. Finally, after a four-night stay at BC Children’s Hospital in Vancouver, she got a diagnosis: acute anxiety.
An honor student, Sue is thin, dark-haired and lily pale. (Her parents requested a pseudonym to protect her privacy.) When a doctor recommended hypnosis, she balked at first. “I thought of it as black magic, like witchcraft,” she says. But neither breathing exercises, nor anti-depressants, had taken away the pain.
So, in early September, she visited Dr. Leora Kuttner, a pediatric psychologist who specializes in clinical hypnosis, a technique for leveraging the brain’s healing abilities during a trance state.
Kuttner’s office has a rumpus-room feel, with toys, plants and colorful pictures scattered about. Settling into a plump beige armchair by the window, Sue breathed slowly as the psychologist asked her to “go to a quiet place.” She chose a beach. Then, in a soft, soothing voice, Kuttner suggested that she imagine a “protection skirt” that could shield her from stomach pain.
Sue pictured herself covered in “a golden, shimmery, transparent cocoon, floating up in the air above this beach.” For a few moments, she felt as though she had left the room. When Kuttner called her out of her reverie, “I was surprised where I was.” Another surprise: the pain was gone.
Sue keeps a recording of her “protection skirt” hypnosis handy on her phone – all 5 minutes, 56 seconds of it. She is still learning to keep anxiety at bay, but if the abdominal pain ever comes back, she says, “I know how to deal with it.”
Hypnosis isn’t just for hucksters and Hollywood villains any more. Neuroscience studies have shown that this mind-body therapy affects the brain in extraordinary ways. Clinical trials have demonstrated its effectiveness in treating anxiety, phobias, skin rashes, irritable-bowel syndrome and acute and chronic pain.
In France and Belgium, anesthesiologists are offering hypnosis combined with local anesthetic as an alternative to general anesthesia in surgery. In North America, medical centers such as the Mayo Clinic have added hypnosis to their pain-management tools.
Hypnosis doesn’t work for everyone, notes Dr. Amir Raz, Canada Research Chair in the cognitive neuroscience of attention at McGill University and the Jewish General Hospital in Montreal. But “in my opinion, it’s completely underused.”
That may be changing, especially in pediatrics. Over the past four years, Kuttner has been invited to teach hypnosis at the Mayo Clinic, Alberta Children’s Hospital in Calgary and the Hospital for Sick Children in Toronto. Kuttner, who developed her techniques more than three decades ago, says she’s “thrilled” by the uptake.
As with mindfulness meditation, hypnosis harnesses the brain’s natural abilities to regulate the body and control the random thoughts that ricochet through our minds, says Dr. David Patterson, a University of Washington psychologist who has studied hypnosis since the 1980s, in a series of clinical trials financed by the U.S. National Institutes of Health.
But, he adds, meditation can take weeks or months of practice before it helps patients dial down pain. With hypnosis, “the relief is just a lot quicker and more dramatic.”
Hypnosis reduces our awareness of what’s going on around us, even as it increases our attention and openness to new ideas. The brain’s  command center lets its guard down, allowing the therapist’s suggestions to embed themselves into the parts of our grey matter that regulate our thoughts, perceptions and physiology, Patterson says. “It’s as if you’re talking directly to the brain.”
command center lets its guard down, allowing the therapist’s suggestions to embed themselves into the parts of our grey matter that regulate our thoughts, perceptions and physiology, Patterson says. “It’s as if you’re talking directly to the brain.”
At Legacy Oregon Burn Center in Portland, Ore., Dr. Emily Ogden, a psychologist, uses hypnosis to help patients cope with the most excruciating injuries you can have.
In the facility’s bedroom-sized intensive-care units, machinery for monitoring vital signs beeps nonstop as nurses and doctors cut away layers of clothing and scorched flesh. The air is putrid-sweet, the smell of open wounds.
Often, the pain of the burn itself pales next to the agony of having dead tissue removed in a process called debridement, or a patch of healthy skin shaved and grafted onto a wound. Then there are the dressing changes. Every day or so, nurses replace fluid-soaked gauze to prevent a burn victim’s greatest threat: infection. The sudden gust of cold air on exposed wounds can be torturous, even with painkillers.
Burn patients tend to be open to hypnosis, Ogden says, but they often add something such as, “I’m not going to squawk like a chicken, am I?”
After reassuring them that no, she won’t make them cluck, Ogden stands by the bedside and asks the patient to imagine stepping down a flight of stairs as she counts backward from 20. Once the patient is deeply relaxed, she gives a series of hypnotic “suggestions,” or instructions for the brain.
For example, “When a nurse touches you on the shoulder, you will return to the feeling of relaxation you have now,” she might say. “During the procedure, you will have no feelings other than comfort and relaxation. Later, you’ll be surprised at how easily it goes for you.”
As simple as it sounds, the technique usually works, says Ogden, who began offering hypnosis six months ago. “It has proven to be such a beneficial and effective intervention.”
Hypnosis stimulates specific brain activity, according to a 2016 study from Stanford University. Researchers found three brain changes in adults who scored high in susceptibility to hypnosis and these changes occurred only while they were hypnotized.
Using a brain-imaging technique called fMRI, researchers found decreased activity in the brain’s salience network, the inner “air-traffic controller” that processes stimuli and preps us for action.
Secondly, they saw greater connectivity between the brain’s executive-control network and the insula, a grape-sized region deeper in the brain that helps us “control what’s going on in the body, and process pain,” the study’s co-author, psychiatrist Dr. David Spiegel, says.
Finally, the researchers observed reduced connections between the executive-control center and the “default-mode” network, involved in self-reflection. This could lead to a disconnect between a person’s actions and their awareness of their actions, Spiegel says.
He describes hypnosis as a “very powerful means of changing the way we use our minds to control perception, and our bodies.” If more practitioners had training to use it, hypnosis could make “a huge difference” in the opioid epidemic, he adds.
In a previous study, published in The Lancet, Spiegel and colleagues instructed patients in self-hypnosis techniques before they underwent vascular or kidney procedures.
Compared with patients receiving standard care, the hypnosis group used significantly less pain medication (fentanyl and midazolam). Spiegel’s team is now testing the same approach in knee- and hip-surgery patients.
He notes that the risk of addiction increases when people are on opioid painkillers for more than three days. If patients can get through the post-surgical period faster, “you can prevent them from getting hooked.”
 But hypnosis has an image problem. Unlike mindfulness, it lacks Zen-master cachet. Doctors and patients have trouble forgetting the dangling pocket watches of stage hypnosis, or the bad guys who put sleeper agents under “mind control” in movies such as The Manchurian Candidate.
But hypnosis has an image problem. Unlike mindfulness, it lacks Zen-master cachet. Doctors and patients have trouble forgetting the dangling pocket watches of stage hypnosis, or the bad guys who put sleeper agents under “mind control” in movies such as The Manchurian Candidate.
Despite solid evidence from clinical trials, the medical field’s approach to hypnosis has been “extremely careful and conservative,” Raz says.
And let’s face it: For every credible scientist studying hypnosis, there are hundreds of charlatans touting self-hypnosis CDs or sessions on Skype as a miracle cure for everything from obesity to cancer. In the land of psychics and crystal magic, anyone can become a “certified hypnotherapist” in a month or less. Rampant quackery “gives us a bad name,” Patterson says.
Adults tend to insist they are impervious to hypnosis, even if they’ve never tried it, Raz says. They think of it as “feeble-mindedness, or the ability to be manipulated.”
But in fact, people who respond to hypnosis may have better co-ordination between brain areas that “integrate attention, emotion, action and intention,” according to a 2012 study published in the Archives of General Psychiatry.
About 10 to 15 percent of adults are “highly hypnotizable,” meaning they can easily slip into a trance and act on hypnotic suggestions. The same percentage of adults do not respond to hypnosis at all, while the rest are somewhere in between. The trait may be genetic, researchers say. But imagination also plays a role.
Responsiveness to hypnosis reaches its peak between the ages of 8 and 12, says Kuttner, who began using hypnosis in the mid-1980s to help children cope with pain in the oncology ward at BC Children’s Hospital.
She documented her techniques in No Tears, No Fears, a short film featuring eight kids with cancer, aged 3 to 12. Guided by Kuttner, the children went through procedures such as spinal taps with only local anesthetic at the needle site. (At the time, general anesthesia in children was reserved for special circumstances, such as major surgery.)
Most children can easily imagine an invisible “magic glove” that keeps needles from hurting, or a fantasy world free of pain, Kuttner says. Concentrating on these beliefs can have analgesic effects. With a fond smile, she recalls a child with leukemia who spent her treatments in an imaginary land of candy.
A more recent patient, 17-year-old Isabella Hay, says working with Kuttner helped her overcome muscle twitches and symptoms of obsessive-compulsive disorder. Starting at the age of 4, Isabella learned to visualize entering a room and turning off switches that controlled her nervous ticks.
When Isabella received a diagnosis of OCD at the age of 13, Kuttner taught her how to focus on her breathing and picture herself in calm place, using a form of self-hypnosis. The technique has given her control over compulsive behaviors, such as a need to touch a rock a certain number of times, Isabella says.
She used to feel panicky at the idea of sleeping away from home. Now, she is graduating from high school with acceptance letters from both the University of British Columbia and Queen’s University. Knowing that the brain is strong enough to “transport you from the thoughts,” Isabella says, “I feel more secure and confident, and less vulnerable in my own head.”
Hypnosis techniques are relatively easy for health-care professionals to learn, Kuttner says. But like other specialists interviewed for this article, she cautions patients against seeking hypnosis from someone with no medical training. “Things can go haywire.”
A lay hypnotist could fail to recognize the signs of psychosis, or encourage someone to regress to an earlier life stage filled with traumatic memories, “and they won’t have a clue how to help the person.”
Kuttner recalls treating a patient who had gone to a lay hypnotist for headache relief but came away weeping and confused. Hypnosis needs to be in the hands of “someone who respects it, and knows what they are doing,” she says. “This is powerful stuff.”
In hypnosis circles, the word “powerful” comes up a lot. But it’s hardly an overstatement when you consider the work of Dr. Marie-Elisabeth Faymonville, director of the pain clinic and palliative care at the University Hospital of Liège, Belgium.
Hypnosis allows patients to avoid general anesthesia in surgeries ranging from mastectomies to heart-valve replacements, Faymonville says.
Since 1992, she has treated more than 9,500 surgery patients with “hypno-sedation,” combining hypnosis with small amounts of local 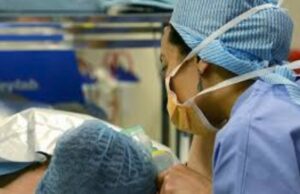 anesthesia. Of those patients, just 18 had to switch to general anesthesia. “It’s really rare,” she says, in German-accented English.
anesthesia. Of those patients, just 18 had to switch to general anesthesia. “It’s really rare,” she says, in German-accented English.
The method appeals to patients who want to be “aware during surgery, but comfortable.” Patients do not get a dry run. Instead, Faymonville assesses their level of motivation and confidence in the surgical team, and their ability to co-operate.
Hypno-sedation works because the patient wants it to work, she says: It’s the opposite of “mind control.” The anesthesiologist’s job is to use hypnotic techniques and communicate with the patient, but the patient must collaborate, “so he puts himself in the hypnotic state.”
She emphasizes that unlike the cross-section of patients you might find in the average hospital, her patients are “highly motivated” to stay conscious during surgery. But in general, she adds, doctors tend to underestimate the resources patients can access with their own minds. “Hypnosis is a talent, a gift from nature.”
THE GIFT OF HYPNOSIS
The ability to be hypnotized is a talent, like an ear for music, researchers say. The easiest way to know if you have it is to give it a try. So, I ask Dr. Lance Rucker, president of the Canadian Society of Clinical Hypnosis, if he’ll hypnotize me.
A dentist by training, Rucker teaches hypnosis to third-year dentistry students at the University of British Columbia, where it’s part of the required curriculum.
Dentists need to learn the basics of hypnosis to “avoid abusing the trance state,” he says. People drift in and out of light trances throughout the day, whether they’re on “autopilot” for the daily commute, or so engrossed in an X-Men flick that they forget it’s a movie.
Dental patients – triggered by memories of needles, drills and frozen-gums past – are often in a daze even before they lie on the chair. When patients are in this vulnerable state, a dentist’s soothing words (“let’s make sure you’re comfortable”) can help make it so. On the flip side, stock phrases such as, “this might hurt a little,” may intensify pain and fear, he says.
Rucker emphasizes that reputable practitioners will not use hypnosis for purposes outside their medical specialty. He asks if I have a dental issue I’d like to resolve. An overactive gag reflex, perhaps? Or a fear of dental fillings?
I am definitely a grinder. That may not be easily fixed, depending on the root cause, he replies. But he’s willing to give it a go.
We sit in the front seats of his scarlet Acura, parked outside a cluster of big-box stores near his home in Burnaby, B.C. The windows are closed to shut out the rumble of traffic and the air is warm and stuffy. I am drowsy already.
In a soft, calm voice, Rucker asks me to take myself to “an internal space, a creative space.” As I relax, he says, my inner awareness can let me know “what it’s all about, and has been all about – the clenching, the grinding.”
A symbol or realization may come to mind. He pauses for a few moments. Then he suggests that I ask my inner self whether it can let the grinding go, “or whether there is some part of you that may wish to hold on to it.”
As his voice meanders, I have a clear picture of a big black dog with massive metal jaws. Could my clenching be a hard-wired defense mechanism? It’s an obvious symbol. But as it turns out, my inner guard dog refuses to back down easily. Later that day, my jaw feels as tight as ever.
A life-long grinding habit could be a problem that a single session in a parked car cannot solve. I might give hypnosis another try. But maybe I just don’t have the gift.
By: Adrianna Barton

 Virtual reality hypnosis (VRH) can reduce the need for postoperative opioids and anti-anxiety medications and lead to improved outcomes in children, new research suggests.
Virtual reality hypnosis (VRH) can reduce the need for postoperative opioids and anti-anxiety medications and lead to improved outcomes in children, new research suggests.
A team of anesthesiologists at the University of Texas Southwestern Medical Center and Hopitaux Universitaires de Strasbourg in France studied 21 children undergoing surgery for scoliosis, comparing 10 who received VRH in addition to the usual postoperative pain management to 11 children who did not receive VRH.
They found that the VRH group had significantly lower need for supplemental treatment for anxiety, opioid analgesics, and less incidence of vomiting as well as shorter time to urinary catheter removal and shorter time to getting up.
“Nonpharmacological approaches should play a critical role in treatment of perioperative anxiety and pain,” corresponding author Girish P. Joshi, MD, professor of anesthesiology and pain management, University of Texas Southwestern Medical Center, Dallas, told Medscape Medical News.
“This can be achieved through several approaches, including appropriate/adequate education and discussion, as well as use of novel technology,” he said. The study was presented at Anesthesiology 2018, the annual meeting of the American Society of Anesthesiologists in San Francisco.
Encouraging Findings
“Hypnosis and virtual reality (VR) have been shown to influence anxiety and chronic pain, but its role in acute pain, particularly in children, was not assessed previously,” Joshi said.
The aim of the current retrospective study was to evaluate the effects of VRH support on postoperative pain and opioids use in children undergoing scoliosis surgery.
From May 2017 onward, VRH support was added to the usual postoperative pain management in all pediatric patients, with a VRH session performed daily for 20 minutes during the first 72-hour postoperative period.
The control group consisted of children who had undergone the same procedure without VRH support before May 2017 and were demographically similar to the VRH group.
The researchers collected data regarding maximum postoperative pain scores per day, the total opioid dose, the number of postoperative vomiting episodes, request for supplemental treatment for pain and/or anxiety, time to oral intake, time to urinary catheter removal, time to getting up, and hospital length of stay.
The VRH group experienced several significant advantages over the control group:
- Only 20% of the VRH group required opioid medication, compared with 62.5% of the control group (P = .15)
- Only 37.5% of the VRH group required anti-anxiety medication, compared with 100% of the control group (P = .04)
 Total postoperative morphine consumption over the 72-hour period was almost twice as high in the control group vs the VRH group (2.15 mg/kg [1.11] vs 1.18 mg/kg [0.28] P = .015)
Total postoperative morphine consumption over the 72-hour period was almost twice as high in the control group vs the VRH group (2.15 mg/kg [1.11] vs 1.18 mg/kg [0.28] P = .015)- VRH group members were able to get up more quickly after surgery, compared to the control group (23 hours [3] vs 44 hours [16.02] P = 0.004)
- The VRH group experienced less postoperative vomiting, compared to the control group (40% vs 83.33%, P = .15)
- Time to catheter removal in the control group was twice that of the VRH group (40.95 hours [18.1] vs 20.14 hours [8.9] P = .03)
- There was no significant difference in average length of stay between the control and the VRH groups (137.7 hours vs 125.5 hours).
- “To our knowledge, this is the first study assessing the postoperative use of VRH in children,” the authors write. “These findings of this pilot study are encouraging.”
- Joshi emphasized that before this technology can be implemented in current routine clinical practice, more prospective, randomized controlled trials that are “adequately powered” are needed.
- Creative, Useful
- Commenting on the study for Medscape Medical News, David Spiegel, MD, Willson Professor in Medicine and Associate Chair of Psychiatry at Stanford University in California, said that although it was not a controlled trial, it was nevertheless “very compelling” and described VRH as “a very creative and useful technique.”
- “Particularly notable is that the children given the VRH used half the opioid dose,” pointed out Spiegel, who was not involved with the study.
- “These days, 133 people per day in the US are dying of opioid overdoses and the longer you stay on them [opioids] the more likely you are to become addicted, especially
 since these are children and not adults.”
since these are children and not adults.”
- “So anything that can reduce opioid consumption — both the amount and the length — is protective, and one way to look at VRH is that it seems to help and it sure doesn’t hurt,” he added.
- Spiegel noted that, as a group, children are more easily hypnotized than adults.
- He referenced a study that he and four colleagues conductedin 2005, in which children undergoing voiding cystourethrography, an invasive and painful procedure involving insertion of contrast dye into the bladder, were randomized to 2 groups: half received routine care, including hospital-provided recreation, while the other half received a hypnosis intervention.
- “We were able to reduce pain and distress and shorten the procedure time by 17 minutes in the hypnosis group,” he reported.
- The current study is “consistent with these findings, and the combination of VRH is interesting since VR helps to do technologically what one does phenomenologically in hypnosis — in other words, narrowing the focus of attention.”
- He hopes that the VRH study “sets a precedent for support like this for children routinely when they undergo procedures like this.”
- Joshi added that the Strasbourg group is contemplating a prospective study.
- “We are hoping other groups will also embark upon research similar to ours,” Joshi said.
- No source of funding for the discussed VRH study was disclosed by its authors in the original article. Joshi, study coauthors, and Spiegel have disclosed no relevant financial relationships.
- Anesthesiology 2018 from the American Society of Anesthesiologists: Abstract Presented October 14, 2018.
- For more from Medscape Neurology, join us on Twitter and Facebook
By: Batya Swift Yasgur, MA, LSW

 In an effort to evaluate the reduction of emotional and physical disturbances in patients scheduled for breast biopsy, this study compared audio-recorded hypnosis with background music vs. music without hypnosis. It also included a control group.
In an effort to evaluate the reduction of emotional and physical disturbances in patients scheduled for breast biopsy, this study compared audio-recorded hypnosis with background music vs. music without hypnosis. It also included a control group.

 Doctors and researchers at MD Anderson are exploring hypnosedation to manage pain and anxiety during certain breast cancer surgeries.
Doctors and researchers at MD Anderson are exploring hypnosedation to manage pain and anxiety during certain breast cancer surgeries. “Do you have a place where you feel really comfortable and at ease?” Engle asked Levinson in her soothing, mellifluous voice. “It could be your grandmother’s house.
“Do you have a place where you feel really comfortable and at ease?” Engle asked Levinson in her soothing, mellifluous voice. “It could be your grandmother’s house.
 They can guide themselves. They can walk through this experience with surgery and take it throughout the treatment process, the whole continuum of cancer care.”
They can guide themselves. They can walk through this experience with surgery and take it throughout the treatment process, the whole continuum of cancer care.”

 Last summer, at age 14, Sue Jones suffered from stabbing pains in her abdomen that got so intense, “I couldn’t walk.”
Last summer, at age 14, Sue Jones suffered from stabbing pains in her abdomen that got so intense, “I couldn’t walk.” command center lets its guard down, allowing the therapist’s suggestions to embed themselves into the parts of our grey matter that regulate our thoughts, perceptions and physiology, Patterson says. “It’s as if you’re talking directly to the brain.”
command center lets its guard down, allowing the therapist’s suggestions to embed themselves into the parts of our grey matter that regulate our thoughts, perceptions and physiology, Patterson says. “It’s as if you’re talking directly to the brain.” But hypnosis has an image problem. Unlike mindfulness, it lacks Zen-master cachet. Doctors and patients have trouble forgetting the dangling pocket watches of stage hypnosis, or the bad guys who put sleeper agents under “mind control” in movies such as The Manchurian Candidate.
But hypnosis has an image problem. Unlike mindfulness, it lacks Zen-master cachet. Doctors and patients have trouble forgetting the dangling pocket watches of stage hypnosis, or the bad guys who put sleeper agents under “mind control” in movies such as The Manchurian Candidate. anesthesia. Of those patients, just 18 had to switch to general anesthesia. “It’s really rare,” she says, in German-accented English.
anesthesia. Of those patients, just 18 had to switch to general anesthesia. “It’s really rare,” she says, in German-accented English.
 Virtual reality hypnosis (VRH) can reduce the need for postoperative opioids and anti-anxiety medications and lead to improved outcomes in children, new research suggests.
Virtual reality hypnosis (VRH) can reduce the need for postoperative opioids and anti-anxiety medications and lead to improved outcomes in children, new research suggests. Total postoperative
Total postoperative  since these are children and not adults.”
since these are children and not adults.”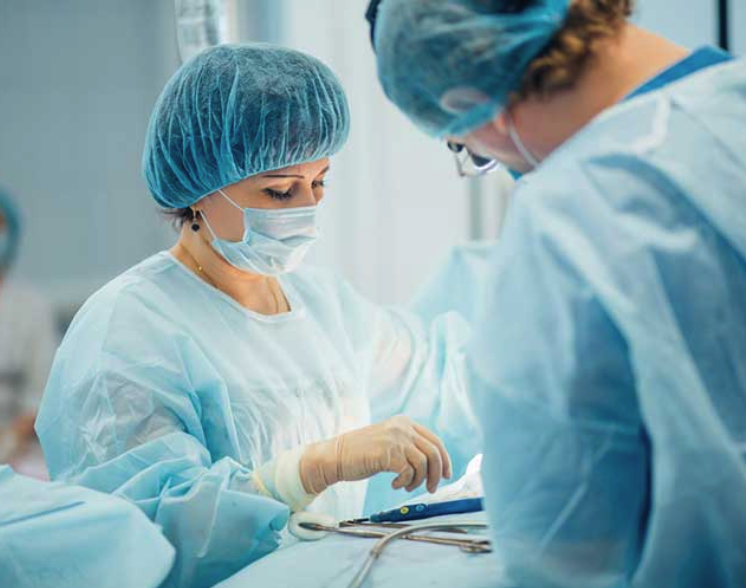
 Clinical hypnotherapy has been gradually gaining momentum in the medical mainstream as a legitimate tool supporting healthy change. I have been in practice since 2001, and in the past 5 years the number of clients looking for help related to medical conditions has grown significantly.
Clinical hypnotherapy has been gradually gaining momentum in the medical mainstream as a legitimate tool supporting healthy change. I have been in practice since 2001, and in the past 5 years the number of clients looking for help related to medical conditions has grown significantly.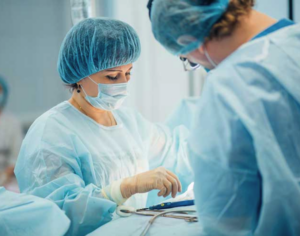
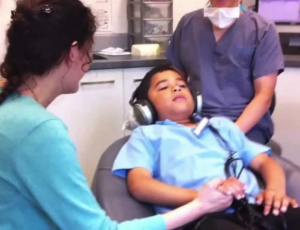 This study also reported that the hypnosis group saved $772/patient mainly due to reduced surgical time. These patients also required less analgesic lidocaine and the sedative propofol during surgery. (Journal of the National Cancer Institute 2007)
This study also reported that the hypnosis group saved $772/patient mainly due to reduced surgical time. These patients also required less analgesic lidocaine and the sedative propofol during surgery. (Journal of the National Cancer Institute 2007)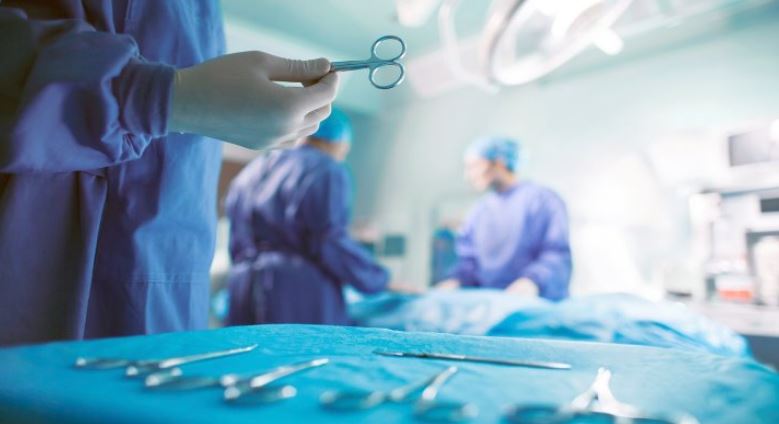
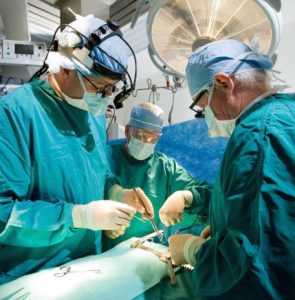 Hypnosis has been used for centuries for pain control, including during the Civil War when Army surgeons hypnotized injured soldiers before amputations. Recent studies have confirmed its effectiveness as a tool to reduce pain.
Hypnosis has been used for centuries for pain control, including during the Civil War when Army surgeons hypnotized injured soldiers before amputations. Recent studies have confirmed its effectiveness as a tool to reduce pain.







